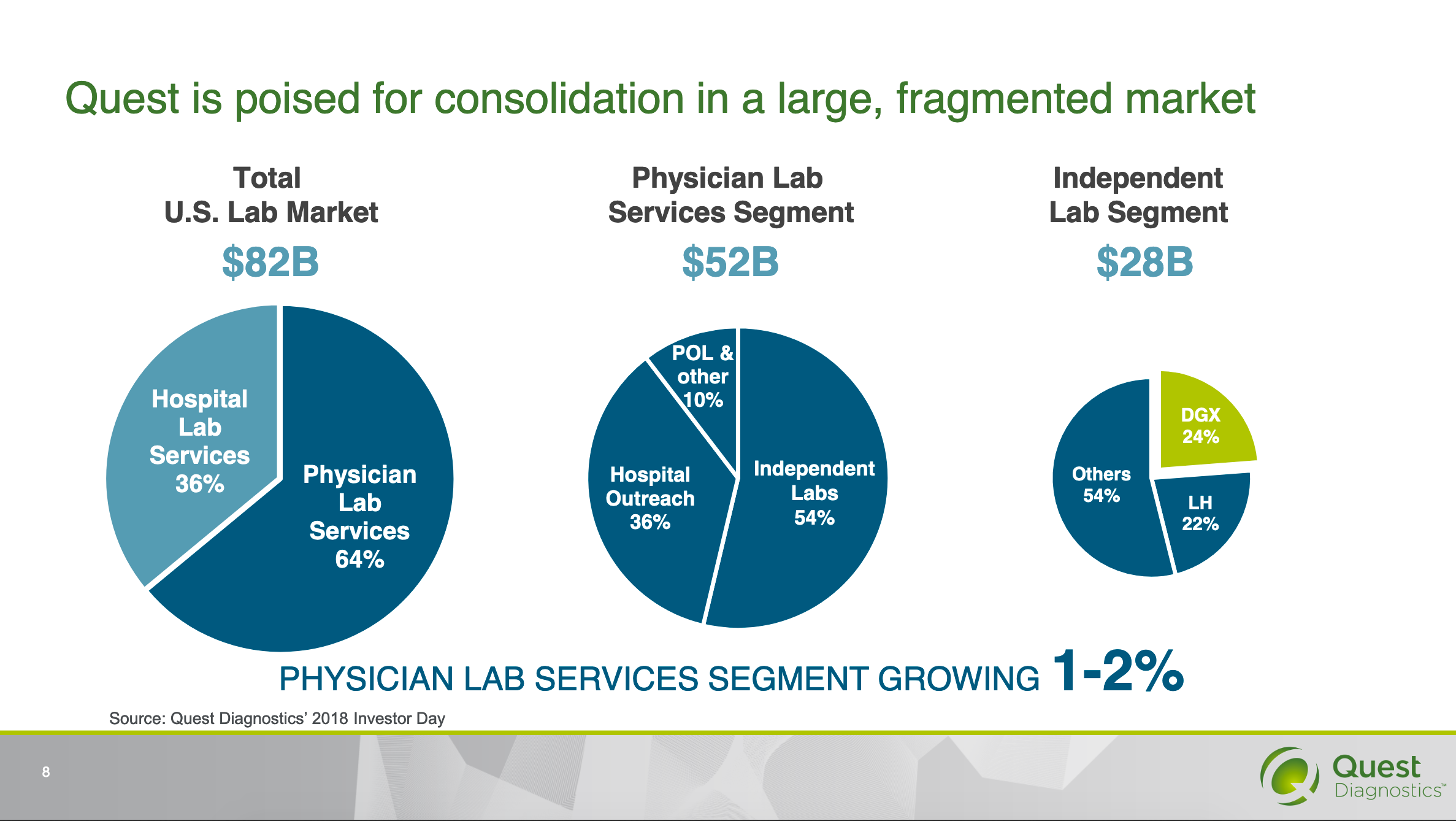
In order to determine the baseline aneuploidy screen uptake rate at NHGB, we performed a chart review of all subjects receiving prenatal care at the facility from Januthrough December 31, 2018. Inputs for the analysis included the population aneuploidy screen uptake rate, upfront costs of the two screening methods, test performance characteristics, travel expenses, consultative services, evaluation and follow-up testing of an abnormal screen result, and lost productivity. 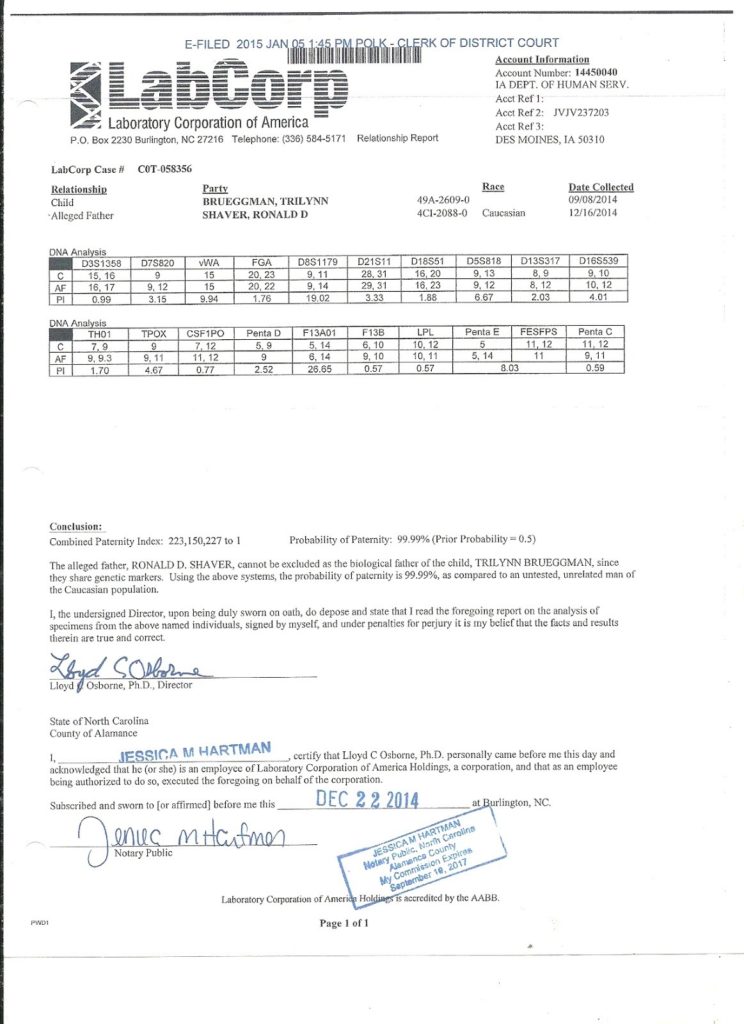
22, 23 For the analysis, we used a theoretical cohort of 100 patients, which corresponds to the delivery volume at NHGB for a 5- to 6-year period. We selected NHGB as a surrogate for an austere clinical environment and performed a prenatal cost of care analysis comparing traditional 2-part serum screening to cfDNA for trisomies 18 and 21. This protocol was approved by the Institutional Review Board at Naval Medical Center Portsmouth (Portsmouth, VA, USA). We hypothesized that despite higher upfront costs, cfDNA might prove more economical in this austere environment when factoring in secondary costs. The objective of this study was to compare the direct and indirect prenatal costs of traditional 2-part serum-based screening to cfDNA for detection of trisomies 18 and 21 at this location. Although prior cost analyses demonstrate a clear benefit to screening for trisomy 21 in general and the use of cfDNA in high-risk patient populations, 21 evidence on the optimal screening strategy in an austere environment is limited. 20 As a result, many labs and patients requiring evaluation of an abnormal screen result must be transported off island to the continental United States. 
19 The facility lacks onsite genetic counseling and Maternal-Fetal Medicine consultative services and has limited laboratory and radiology capabilities. 18 The hospital has a staff of about 250 personnel (with a single obstetrician) serving an installation population of 6,000. military installation located on a strip of land (approximately 115 square kilometers) in eastern Cuba. Naval Hospital Guantanamo Bay (NHGB) is an example of an austere clinical environment. Despite more limited resources, research suggests that some austere clinical locations may rely on inferior screening tests compared with their more resource-rich counterparts. The upfront costs of screening must be balanced with these secondary expenses. 14–16 There are several unique considerations for these environments, such as transportation of tests to offsite labs, travel to a tertiary medical center for evaluation of an abnormal screen result, and the clinical implications of unrecognized aneuploidy at birth in a resource-limited setting. 1, 13Īustere clinical environments include practices providing care in resource-limited locations such as underserved urban areas, rural areas, disaster zones, some Native American/Aborigine/First Nations communities, and military installations in remote locations. Initial societal guidelines recommended cfDNA for high-risk pregnancies 12 but more recently favor an individualized approach with the option of traditional screening with or without sonographic assessment of nuchal translucency or cfDNA for pregnancies across the risk spectrum. 9–11 However, it has significantly higher upfront costs. 8 Noninvasive prenatal testing has a higher detection rate for trisomy 21 than traditional screening approaches and offers screening for other common autosomal and sex chromosomal aneuploidies and more recently subchromosomal microdeletions and duplications. 7 It incorporates DNA fragments released into the maternal plasma from apoptotic cells from the pregnancy. 2–6Ĭell-free DNA (cfDNA) also known as noninvasive prenatal testing or “NIPT” is a more recent technology that became available in clinical practice around 2011. 1 Traditional screening encompasses a variety of tests incorporating serum analytes, and in some cases sonography, with varying detection and false-positive rates. Screening and diagnostic testing for major chromosomal abnormalities including an abnormal copy number (termed “aneuploidy”) should be offered to all women in early pregnancy-ideally at the first prenatal visit.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
